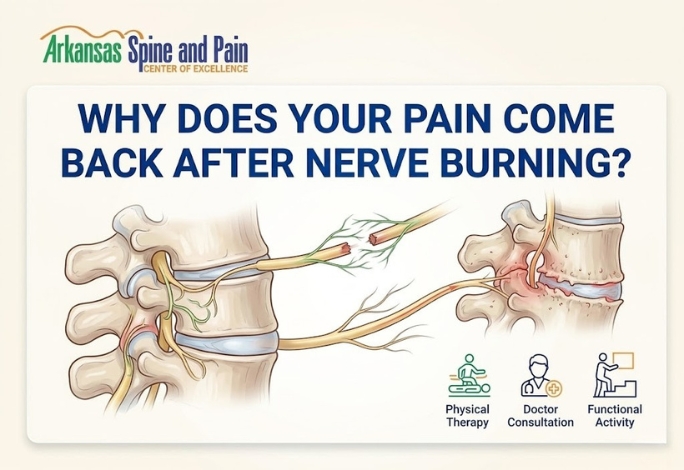
Radiofrequency ablation (RFA), often referred to as “nerve burning,” is a highly effective interventional treatment for chronic neck, back, and joint pain. For many patients at Arkansas Spine And Pain, this procedure provides months or even years of profound relief. However, a common question arises when discomfort gradually returns: why isn’t the relief permanent? Understanding the biological process of nerve regeneration and the mechanics of pain signals is essential for managing long-term expectations and maintaining a high quality of life.
The Biological Reality of Nerve Regeneration
The most straightforward reason pain returns after a successful ablation is that nerves are living tissue designed to heal. During an RFA procedure, thermal energy is used to create a lesion on the specific sensory nerve responsible for transmitting pain signals from a joint to the brain. While this “interrupts” the signal, it does not destroy the nerve’s ability to regrow.
Over time, the treated nerve undergoes a natural regenerative process. Microscopic nerve fibers slowly bridge the gap created by the thermal lesion. Once the nerve connection is re-established, it resumes its role of sending sensory data. When this happens, the original pain sensations typically return. This isn’t a failure of the procedure; rather, it is a testament to the body’s resilient healing mechanisms. On average, patients experience relief for six to eighteen months before this regeneration necessitates a follow-up consultation with a Pain Management doctor in Arkansas to discuss repeating the treatment.
Structural Changes and New Pain Sources
While nerve regrowth is the primary culprit, it is not the only reason you might feel discomfort again. The human body is a complex system of interconnected parts, and chronic conditions like osteoarthritis or degenerative disc disease are often progressive. Even if the specific nerve that was “burned” remains dormant, the underlying structural issue such as a worn facet joint or a bulging disc continues to exist.
As these conditions evolve, they may begin to irritate adjacent nerves that were not included in the original ablation. In these instances, the “new” pain might feel very similar to the old pain, leading patients to believe the procedure has worn off. A comprehensive diagnostic approach is required to determine if the original nerve has regrown or if a new area of the spine requires attention. Maintaining a relationship with a specialized clinic ensures that these shifts in your pathology are caught early and treated with precision.
The Role of Lifestyle and Physical Therapy
The success of interventional pain management is often tied to what happens after the patient leaves the clinic. Nerve burning provides a “window of opportunity” where pain is significantly reduced, allowing the patient to engage in physical therapy and strengthening exercises that were previously too painful to perform.
If a patient remains sedentary during the months of relief, the muscles supporting the spine may weaken further. This lack of structural support puts additional stress on the joints and nerves. Consequently, when the nerve eventually regrows, the pain may return more intensely because the surrounding physical framework has deteriorated. Utilizing the pain-free period to build core strength and improve posture is the best way to extend the functional benefits of any interventional procedure.
Understanding Procedural Variations and Accuracy
Not all nerve burning procedures are identical. The effectiveness and duration of relief depend heavily on the accuracy of the initial diagnostic blocks and the precision of the electrode placement during the ablation. If the thermal lesion does not fully encompass the targeted nerve, the interruption of the pain signal may be incomplete, leading to a faster return of symptoms.
This is why image guidance, such as fluoroscopy, is a non-negotiable standard for modern interventional care. By using real-time X-ray imaging, specialists can ensure the heat is applied exactly where it needs to be. Furthermore, individual anatomy varies; some people have accessory nerves that provide “backup” pathways for pain. If these variations aren’t accounted for, the relief might feel shorter than expected. Honesty regarding the duration of relief helps patients and providers work together to refine the approach for future sessions.
Managing Expectations for Chronic Pain
It is important to view radiofrequency ablation as a powerful tool for management rather than a permanent “cure.” For those dealing with chronic spinal conditions, the goal is often to reduce the “pain load” to a level where daily activities, work, and sleep are no longer a struggle.
Because RFA is minimally invasive and carries a low risk of complications compared to major surgery, it can be repeated safely once the nerves regrow. Many patients find that incorporating RFA into a broader treatment plan which might include lifestyle adjustments and non-opioid medications provides the most consistent results. By staying informed about how the body heals and staying proactive with clinical check-ups, patients can successfully navigate the cycle of chronic pain and maintain their independence.
Frequently Asked Questions
Is nerve burning a permanent solution for back pain?
Nerve burning, or radiofrequency ablation, is not permanent because nerves naturally regrow over time. Most patients experience relief for 6 to 18 months, after which the procedure can usually be repeated to restore pain relief.
How long does it take for nerves to regrow after RFA?
The rate of nerve regeneration varies by individual, but typically it takes between six months and a year and a half for the treated nerve to fully recover and begin transmitting pain signals to the brain again.
Why did my pain return only two months after the procedure?
If pain returns quickly, it may be due to incomplete lesioning of the nerve or the presence of additional “accessory” nerves. In some cases, a new, different source of pain in the same area may be the cause of the discomfort.
Can the RFA procedure be repeated safely?
Yes, radiofrequency ablation is considered safe to repeat once the original relief has worn off and the nerve has regrown. Many patients incorporate periodic RFA treatments into their long-term chronic pain management plan.
Will the pain be worse when the nerve grows back?
Typically, the pain returns to its original baseline level. However, if the underlying condition like arthritis has progressed in the interim, the sensation might feel different or more intense than it was prior to the initial treatment.
Is nerve burning the same as surgery?
No, nerve burning is a minimally invasive, outpatient procedure performed with a needle and local anesthetic. Unlike surgery, it does not involve large incisions or a long hospital stay, and recovery time is generally very short.
What are the signs that the nerve is regrowing?
The most common sign is the gradual return of the specific pain you had before the procedure. You may notice a slow increase in stiffness or aching in the treated joint that becomes more consistent over several weeks.
Can lifestyle changes prevent the pain from coming back?
While you cannot stop a nerve from regrowing, improving core strength and flexibility through physical therapy can reduce the mechanical stress on your joints, potentially making the pain more manageable when the nerve does recover.
Are there risks to repeating the nerve burning procedure?
When performed by experienced specialists using image guidance, the risks are minimal. The most common side effects are temporary soreness at the injection site or localized swelling, which usually resolve within a few days.
Why do I need a referral for this treatment?
A referral ensures that a primary doctor has already evaluated your condition and ruled out other issues. This allows the pain specialist to focus on providing the most appropriate interventional treatment for your specific diagnosis.