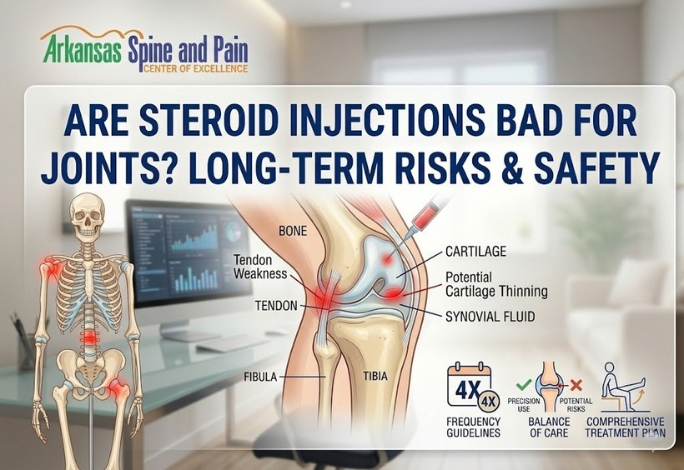
For many people living with chronic inflammation or debilitating arthritis, a corticosteroid shot feels like a miracle. Within days, the sharp, grinding pain in a knee or shoulder often subsides, allowing for a return to daily activities. However, as the initial relief becomes a memory, a common question arises among patients in Arkansas: are these injections doing more harm than good in the long run?
At Arkansas Spine And Pain, we believe that transparency is the foundation of effective care. Steroid injections are a powerful medical tool, but like any intervention, their value depends entirely on how and how often they are used. Understanding the biological impact on your cartilage and tendons is essential for making an informed decision about your joint health.
The Role of Corticosteroids in Pain Management
Corticosteroids are synthetic versions of cortisol, a hormone your body naturally produces to manage stress and inflammation. When injected directly into a joint space, they work by suppressing the immune response and calming the chemical signals that cause swelling and pain. This targeted approach is often superior to oral medications because it delivers the “fire extinguisher” directly to the “fire” without the systemic side effects of high-dose pills.
A Joint Injection is typically recommended when a patient experiences an acute flare-up that hasn’t responded to rest or physical therapy. The goal is rarely to “cure” the underlying condition, such as osteoarthritis, but rather to break the cycle of pain. By reducing inflammation, patients can often engage more effectively in rehabilitation exercises that strengthen the muscles supporting the joint.
Assessing the Long-Term Impact on Cartilage
The primary concern regarding repeated steroid use is its effect on articular cartilage, the smooth, slippery tissue that covers the ends of your bones. Recent clinical studies have suggested that high-frequency injections may contribute to the thinning of this cartilage over several years.
Research published in the Journal of the American Medical Association (JAMA) highlighted that patients receiving repeated injections every three months showed slightly more cartilage loss compared to those receiving a saline placebo. This doesn’t mean a single injection is “bad,” but it does underscore why a Specialized Joint doctor in Arkansas will generally limit the number of shots you receive in a single year. We focus on finding the “minimum effective dose” to ensure your long-term mobility isn’t sacrificed for short-term comfort.
When Are Steroid Injections the Right Choice?
Despite the potential risks of overuse, steroid injections remain a gold standard for specific scenarios. They are exceptionally effective for “mechanical” issues where inflammation is the primary driver of disability.
- Acute Bursitis or Tendonitis: When a bursa sac becomes severely inflamed, a single shot can often resolve the issue entirely.
- Osteoarthritis Flares: If you are unable to walk or sleep due to a sudden spike in pain, an injection provides a window of relief to regain function.
- Diagnostic Clarity: Sometimes, an injection is used to confirm that a specific joint is indeed the source of your pain before moving toward other therapies.
The key is balance. At our clinics, we view these injections as a “bridge” to long-term solutions, such as weight management, physical therapy, or regenerative medicine options like PRP (Platelet-Rich Plasma).
Minimizing Risks Through Precision Medicine
The safety of a joint procedure is also heavily dependent on the technique used. Blind injections where a needle is placed based on external landmarks alone carry a higher risk of hitting a tendon or missing the joint space entirely.
To maximize safety, our specialists utilize image guidance, such as ultrasound or fluoroscopy (live X-ray). This ensures the medication is delivered precisely into the intra-articular space, protecting the surrounding soft tissues and tendons from unnecessary steroid exposure. By using these advanced techniques, we can reduce the likelihood of “steroid flare” and ensure the highest possible efficacy for each dose.
A Personalized Path to Recovery
Every patient’s “pain threshold” and biological makeup are different. What works for a high school athlete with a shoulder injury might not be appropriate for a senior managing chronic hip arthritis.
Choosing a treatment plan requires looking at the “whole person” rather than just the X-ray. If steroids are no longer providing lasting relief, it may be a signal that the joint requires a different approach, such as radiofrequency ablation or regenerative therapies. Staying honest about your symptoms and goals allows your medical team to pivot when necessary, keeping your joints healthy for decades to come.
FAQs on Long-Term Steroid Injection Safety
How many steroid injections can I have in a year?
Most specialists recommend a maximum of three to four injections in the same joint within a 12-month period. Exceeding this limit can increase the risk of cartilage thinning and systemic side effects like bone density loss.
Are there alternatives to steroids for joint pain?
Yes, options include viscosupplementation (hyaluronic acid), PRP therapy, and physical therapy. Some patients also find relief through radiofrequency ablation, which treats the nerves sending pain signals rather than the joint itself.
Can a steroid shot cause my pain to get worse?
A small percentage of patients experience a “steroid flare,” which is temporary irritation in the joint lasting 24 to 48 hours. This usually subsides quickly and is followed by the intended anti-inflammatory relief.
Will I feel the results of the injection immediately?
While the local anesthetic provides numbing for a few hours, the steroid medication typically takes two to five days to begin reducing inflammation. Full benefits are usually felt within one to two weeks after the procedure.
Do steroid injections affect blood sugar?
Yes, corticosteroids can cause a temporary spike in blood glucose levels. Patients with diabetes should monitor their levels closely for several days following an injection and consult their primary care physician if needed.
Is the procedure painful?
Most patients report only a mild pinching sensation or pressure. We use a local anesthetic to numb the skin and the path to the joint, and image guidance ensures the needle follows the most efficient, least disruptive route.
Can steroids weaken my tendons?
Frequent injections near or into a tendon can weaken the collagen fibers, potentially increasing the risk of a rupture. This is why precision and image guidance are critical to ensure the medication stays within the joint space.
Do I need a referral for a joint injection at ASAP?
Arkansas Spine and Pain operates as a referral-based practice. This ensures that you have had a preliminary evaluation by a primary care provider or specialist to confirm that interventional pain management is the right next step.
How long does the relief from a steroid shot last?
Relief typically lasts anywhere from three weeks to three months. The duration depends on the severity of the joint damage and how well the patient follows post-injection activity restrictions and physical therapy.
Can I drive home after getting a joint injection?
In most cases, yes. However, if you are receiving an injection in a weight-bearing joint like the hip or if you received any sedative, we recommend having a driver available to ensure your safety following the appointment.